July 23, 2022
Upcoming Changes to Medicaid
Changes are coming to Pennsylvania’s Medical Assistance Program for the HealthChoices Physical Health Plans. Some Physical Health Managed Care Organizations (PH plans) will no longer be available with the introduction of new PH plans. Approximately 500,000 Medical Assistance (MA) consumers (throughout Pennsylvania) must change their current PH plans. Every person currently receiving Medicaid through the HealthChoices Physical Health Plans will be receiving a mailing from DHS regarding these changes.
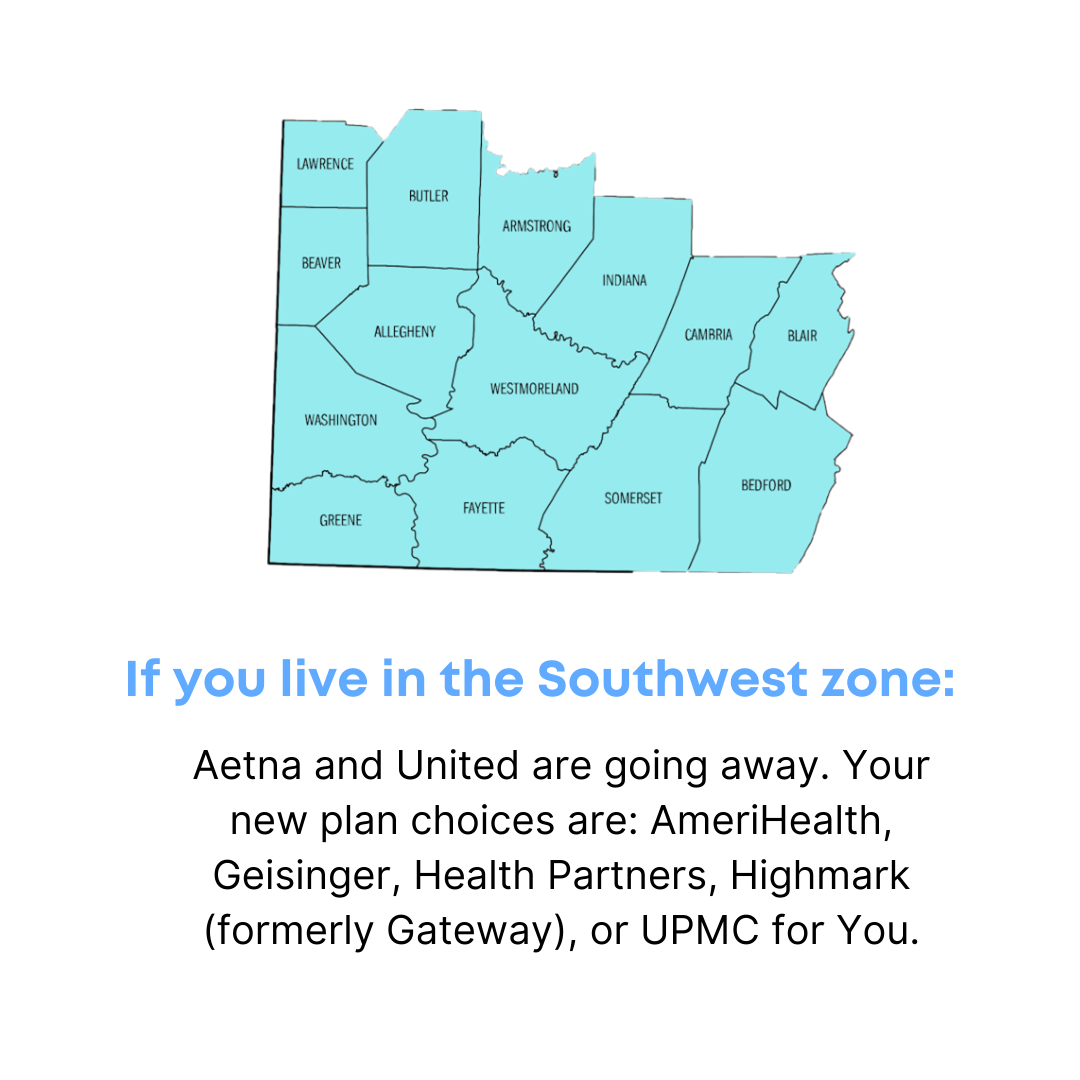
All the counties served by Neighborhood Legal Services (Allegheny, Beaver, Butler, Lawrence) are in the HealthChoices Southwest Zone.
Anyone currently enrolled in the following PH plans will need to select a new Physical Health Managed Care Organization (PH plans)
-
- United Healthcare
- Aetna Better Health
Participants must select a new PH plan between June 22, 2022 through August 16, 2022.
Participants can contact PA Enrollment Services in one of three ways to select a new plan or find out more information about the new PH plans such as doctors, preferred hospitals, and preferred providers covered by these new plans.
-
- Online: enrollnow.net
- Mobile App: PA Enrollment Services
- Telephone: 1-800-440-3989, option 6 to speak with a representative Monday – Friday 8:00 AM to 6:00 PM
- Participants should also receive a notice and comparison chart in the mail
New plans start September 1, 2022.
Some participants will not need to change plans but will have new choices available. If a participant chooses a new PH plan, they will receive a new member ID card in the mail. If a participant must choose a new plan and doesn’t, they will not lose coverage. They will be auto-assigned into a PH plan. If a participant does not need to change PH plans, they are simply given the option to select a new PH plan. These participants do not need to do anything. They will keep their same PH plan.
This does not affect Behavioral Health Plans.
This does not affect Children’s Health Insurance Program (CHIP) participants.
For more information and frequently asked questions click here.